Breastfeeding

Feeding baby is a top stressor for new moms. I don’t need research to tell me that; I’ve seen it first-hand.
The 90’s saw a big resurgence in support of breastfeeding and the message was overwhelmingly clear:
Period. (This would imply that formula-feeding is, in fact, second best.)
I enjoyed breastfeeding both my children into toddlerhood and FULLY support any woman who wants to breastfeed, but I also appreciate the sacrifices that breastfeeding moms make, as well as the fact that unsuccessful breastfeeding can be a traumatic experience for new moms who feel they’ve somehow failed at mothering (already). This result can be devastating.
Let’s back up and start from the beginning:
A Brief History
There’s a decent chance you weren’t breastfed by your own mother. Not too many of us in the past couple generations were. Formula was thought to be a superior food source and breastfeeding was deemed a poor man’s sport. In fact, formula was touted as the best, healthiest food source for babies starting in the early 1900s. For most of the twentieth century, breastfeeding rates in the US were declining.
Thus, our moms were just doing what they were told was best. It wasn’t until second-wave feminism and the women’s health movement of the 1970s that breastfeeding started to (re)gain any kind of popularity. Beginning in the late 80’s and 90’s, breastfeeding started to come back into vogue as mothers, medical professionals, and public health officials alike sought an end to the stigma that had plagued nursing moms in previous decades.
Since then, the “Breast is Best” campaign has gotten the word out and nearly every new mom has gotten the memo. According to the CDC, about 84% of American mothers now breastfeed (for any amount of time), compared with less than two-thirds in 2000.
But have we gone too far? Ask any formula-feeding mom and she will tell you, without a doubt, the answer is YES. But you know what’s funny? Many nursing moms also feel criticism and lack of support for their choice to breastfeed (and pump) from family members (usually older), employers, coworkers, husbands (sometimes), and people in public who are forced to watch them nurse [snort].
So, why is every Tom, Dick, and Harry (Gertrude, Betty, and Sally) SOOOOO interested in how you feed your baby?
We’ll probably never know for sure, but it’s a powerful issue — and one that seems to catch new moms off guard every single time.
*Another thing: Research shows that there are gross racial disparities in breastfeeding practices, driven in large part by systemic barriers to breastfeeding that many minority women face. A better way to put it may be to say that women of color literally do not have the same access to breastfeeding as white women.
To add to the debate, several studies have also shown that breastfeeding perhaps is not as magical as previously thought. As it turns out, previous statistical studies did not control for socioeconomic factors, which more heavily influence the long-term outcomes of children, rather than whether you were fed from the breast or bottle.
- Sibling Study Shows Little Difference Between Breast- and Bottle-Feeding (Time Magazine)
- Is Breast-Feeding Really Better? (NY Times)
- Everybody Calm Down About Breastfeeding (Emily Oster on 538)
- Lactivism, by Courtney Jung
- Bottled Up, by Suzanne Barston
I don’t want to sound like I don’t support breastfeeding. I absolutely do.
I also know there are other benefits of breastfeeding (that aren’t accounted for in these studies), such as weight control for mom, emotional bonding for both mom and baby, and the emotional satisfaction that nursing can bring. It also seems that there are short-term health benefits to breastfeeding for baby, such as better digestion/lower incidences of diarrhea. There’s also some evidence that nursing can lower the risk of certain cancers in mom, namely: breast, endometrial, esophageal, ovarian, thyroid, and uterine cancer.
But does it really matter in the long-term? Will your formula-fed baby be overweight, dim-witted, and uncoordinated? Are you yourself doomed to a cancer diagnosis if you forego nursing? Rest assured that research points to no.
So where does this leave us? I’ll tell you exactly where: knowing you’ll get flak either way, you and your partner get to choose to feed your baby however you want. Everyone else can piss off.
That said, here are some other considerations:
Cost
The reason I choose cost first is simple: for many people, budgets are tight and cost has a dramatic influence on people’s decision-making.
Cost of feeding your baby (for the first 6 months only)
Breastfeeding:
- A pump ($200+) (**Your insurance company should cover one, though it may not be the exact one you desire…)
- A Nursing pillow ($40)
- A Nursing Cover ($35)
- Various other appurtenances (let’s say $50 total)
So, roughly $325. Let’s call it an even $350.
Sound like a lot? Maybe on its face.
Formula:
- About $1,000-$2,000, on average, for formula (annually)
Bottom line: Formula is expensive, y’all.
*This can be a little misleading, though, because it assumes that your time has no value during this time period (i.e., your opportunity cost is zero), which we know is not the case for everyone. If you get paid by the hour, and instead of working, you are spending a lot of time nursing and pumping, obviously this equation changes. And breastfeeding costs do vary widely from one mom to the next — it can get really costly, especially if you’re struggling to nurse.
Onward.
Convenience Factor
It would seem that formula-feeding from a bottle might be much more convenient, right? Yes and no.
As an example, when your newborn wakes up hungry at 3 am (as he will multiple times a night), sticking him on your boob and going back to sleep is waaaaaaay easier than getting up out of bed, trudging down to the kitchen, heating up water and mixing powder, spilling it everywhere, feeding your baby, cleaning the bottles, etc., etc.
Now imagine doing that 2-3 times a night.
The ability to breastfeed at will is also a big help when traveling. There’s usually (though not always, especially if you’re pumping) less to pack, for example. Breastfeeding is also handy on planes, where babies have a very hard time equalizing the pressure in their ears, and suckling relieves that discomfort. (Also: why do babies always seem to need to eat RIGHT NOW when it’s precisely the least convenient time?)
Even if getting on a plane with your baby isn’t at the top of your to-do list, the same basic idea holds true anywhere/time you’re out of your home:
The boob in the mouth is an instant pacifier.
Whether you’re on a park bench, meeting a friend for a walk or coffee, heading to the pediatrician’s office, wherever: if you’re breastfeeding, you can go anywhere you want without carrying around a ton of bottle-feeding gear and coolers and such… all your baby needs is YOU.
This is great, but it can also be VERY burdensome.
I used to observe how my formula-feeding friends’ babies would happily take a bottle from just about anyone; I have to admit it made me a little jealous.
Yes, breastfeeding moms can also pump so that others can bottle-feed their baby, but pumping is time-consuming and burdensome. The fact that anyone can mix a bottle of formula at any time (middle of the night perhaps?) is definitely an advantage.
Nursing Challenges
Again, I absolutely adore breastfeeding, cherish the experience, and would never have done it any differently. That said, it’s not without its battles. Here are the top four complaints you’ll hear from nursing moms:
1. Getting Started Can be Hard
I’m sure you’ve heard many horror stories by now: breastfeeding can be very hard in the beginning. Not only is it exhausting, but a woman whose baby has a bad latch can suffer immensely with cracked, sore, and even bleeding nipples (the rumors are true!). In fact, one study described in TIME Magazine revealed that about half of nursing moms quit within the first few weeks because of difficulties, anxiety, frustration, and lack of support, which is a shame.
But you know what? This will not happen to you because I’m going to tell you *exactly* how to achieve a proper latch (in your Week 39 newsletter, “The Lowdown on Latching” — also summarized below).
2. Really? I’m the only food source?
Especially in the very beginning, the fact that you are the only source of sustenance for your baby can feel incredibly burdensome. Breastfeeding every few hours can be exhausting — no doubt. There are moments when you’ll be like, “Can’t someone else just feed her? Jesus!!”
Your partner might also feel a bit left out because they cannot participate in baby-feeding. This dependence on you as the sole provider can be very stressful for some. For others, it’s a non-issue. And by the time your second baby comes along (if), you probably won’t give it a second thought.
Overcoming It
That’s why God (or… Mr. Medela) invented breast pumps (which, in some ways have evolved quite a bit with technology, and in others, not so much). As soon as your milk comes in, you can pump and store it so that your husband, partner, mom, or even a babysitter can feed your baby to give you a break. In fact, I absolutely recommend you start giving your baby a bottle early(ish) on so she doesn’t reject bottle-feeding in the long-term.
3. The Big 3 Hairy Monsters of Nursing
Most nursing moms will experience one or more of the following three issues at some point in their nursing career: thrush, blocked ducts, and mastitis.
Yeah, it sucks. I’m not gonna lie.
Overcoming It
There is a lot you can do to avoid these. The better educated you are, the better off you’ll be. Keeping your nipples dry and addressing a clogged duct situation before it becomes mastitis — these things are key.
Getting blocked ducts, mastitis, or thrush is a bummer, but it’s nothing you can’t deal with. These can all be treated within a day or two, so it’s really not that bad. Almost everyone has to pay the “breastfeeding tax” at one time or another. It comes with the territory…
4. Pumping at Work Sucks (or, can at least)
If you plan on going back to work in-person before you quit nursing, you’ll have to pump at work.
For many women, this is no big deal, especially if you are an office worker who works for a big company that’s in-the-know about lactation-related laws and such. Perhaps you have a lactation room with complimentary juices and plush club chairs. Consider yourself lucky.
What about a waitress or flight attendant or field worker? Or even a nurse or doctor? Lactation rooms? Yeah, right.
Yes, you could always read the riot act to your boss about your rights as a worker, blah blah blah. But sometimes? It just doesn’t work that way (sadly). In real life, some people are concerned about their job security and don’t want to be that guy.
As the only female employee who was always trying-to-fit-in-with-the-boys at my old job (a general contractor’s office), LET ME TELL YOU – a lactation room? Time off to pump? Putting my telltale bottles of breast milk in the office fridge next to someone’s chicken sandwich? It just wouldn’t happen (sadly). NOPE.
So — it really depends on you and your setup at work. (Read more about pumping at work.)
Overcoming it
If you have a can’t-pump-at-work situation, I tell women all the time: breastfeeding doesn’t have to be an all or nothing thing.
For example, you can nurse your baby in the morning and at night and maybe pump once during the day. Or maybe not pump at all. BF’ing part-time is infinitely better than not BF’ing at all (or quitting very early).
In fact, you can totally customize a feeding plan that works for you and your schedule. Giving breast milk 3x per day and formula 2x per day once you’ve gone back to work is a perfectly manageable solution. That’s just one example.
About 80% of the moms in my prenatal group breastfed for at least 12 months and wouldn’t have changed it for the world (yes, having a support group like this REALLY helps). It was (and continues to be) a wonderful experience that I will always cherish.
Please remember: if you can’t breastfeed, for *whatever* reason, do not beat yourself up about it. We do the best we can, and that’s all anyone can ask of us. #fedisbest
Getting Started
If this is so natural and easy – then why is it so damn hard?? Yes, you will say this to yourself at some point in the beginning. Getting started is not without its challenges, as I’m sure you’ve heard already. I feel there is a certain hump one must get over before really hitting your stride. But don’t worry, with a little persistence and perseverance, you will get there. You WILL get there, mom-eee.
Point being: Almost everyone struggles in the beginning. You are not alone.
In my opinion, the key to a successful start is all in the latch. It’s too bad this isn’t something you can practice at home before the baby arrives, because DAMN it would save a lot of headache. However, you CAN educate yourself:
If your baby has a bad latch, breastfeeding will hurt. A lot.
Start when you are in the hospital: make sure to have the nurses or lactation consultants observe your baby’s latch before you leave.
Essentially, you want your baby’s mouth to be open very WIDE in order to scoop as much of the nipple and areola in as possible. The more boob, the better, people. Depending on your baby, the whole latching procedure requires some precision – like trying to refuel an F-16 mid-air. If your baby’s mouth is not open wide and he is only sucking on the nipple itself, this is where the trouble starts.
How to latch:
- Put on your nursing pillow (in the early days, you may have to use pillows because your Boppy might not fit around your still-bulging belly). Get comfortable and take a deep breath. Find your happy place.
- Have your partner hand you the baby. Put baby on his side, cupping his body around you so he is in the shape of a Capital ‘C.’
- Since he will have no head control, grab the base of his head as shown below:
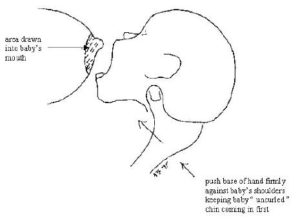
- Bring your baby’s nose to your nipple in order to get him to root around and open his mouth. Some babies do this instantly without hesitation, others need more encouragement. Rub your nipple or finger on baby’s lower lip in order to tease it open (this is where the patience and practice comes in…). WAIT UNTIL BABY’S MOUTH IS WIDE OPEN BEFORE GETTING HIM ON. At all costs. Whatever you need to do to get that mouth open, do that thing. As a practical matter, this part is hard. The reason is because your baby will be crying out of hunger and possibly flailing around. (They don’t show you this part in all the diagrams, WTF.) Your instinct will be to get him latched on as soon as humanly possible because OMAGAH, he is starving – just listen to that wailing(!!) – and I need to get him food, STAT! Resist this urge to rush through it. It’s hard, but resist. Have someone talk you through it to keep your head straight. Remember that baby is not going to die by having to wait an extra 30 seconds to get milk (although it will feel this way).
- When his lower jaw is gaping open, pull him onto your breast, scooping as much of the lower areola in his mouth as possible. Scoop, SCOOP! This is where you will fail or succeed.
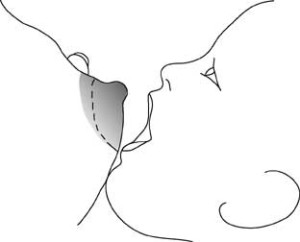
- Ouch, I know. NOW: count backwards from 10 to 1. When your baby first latches on, a little pain is normal. However, if the pain is not improving after you’ve reached 1, you need to start over. This process can be very frustrating and requires a LOT of patience and a little bit of bullet-biting. The problem, you see, is that unlatching your baby can also be painful. Dang, that suck is strong!!! It’s like having a little piranha attached to your boob. NBD.
- To unlatch your baby, wedge your thumb or your pinky into the corner of his mouth or under his lip in order to break the suction. Yes, he will freak out and cry. IT’S OKAY. If he’s latched on poorly, he can cause a lot of damage in a very short amount of time, so do get him off ASAP and try again. Yes, it’s frustrating. You might cry out of pain and/or frustration. It’s okay. This is all normal (sorry). Keep your eyes on the prize. This is what a successful latch will look like (below). You will also know because it won’t be very painful after the first 15 seconds or so.
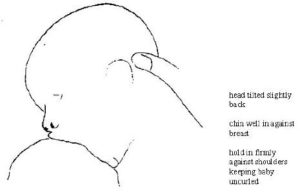
There is so much to say about breastfeeding, but I really wanted to focus on the latch for now. For more information about how to get started breastfeeding, check out La Leche League. Another great reference on getting started is KellyMom.
Next, what I’ve learned about…
Why People Don’t Breastfeed or Quit Prematurely
There are, in my experience, three main reasons why moms give up prematurely on breastfeeding. If you understand this and expect some of these obstacles along the way, you will have a much better chance of long-term success at nursing, which is SO overwhelmingly rewarding.
A. Pain and/or other physical problems
Breastfeeding can be really hard in the beginning. There, I said it. It’s true. Many newborn babies do not latch properly or at all. In more cases than not, you have to guide your baby to a proper latch. Start in the hospital where you have free help. Let the nurses and lactation consultants observe your baby’s latch. If nobody offers this help, you need to ask. Don’t be shy: it’s too important. If you leave the hospital with wounded nipples because of latching problems, your chances of continued breastfeeding are greatly diminished.
Pain is ubiquitous among new nursing moms. However, it should improve over the first couple of weeks. If you get home and can’t manage your pain, call a lactation consultant to come to your home – or attend a free lactation support group (usually offered through your hospital). Please don’t give up before you do this! Some people (like me) need a little extra help getting over the hump.
MANY (most?) moms will go on to develop blocked ducts, mastitis, and/or thrush at some point in their nursing career. These are the Big 3 Hairy Monsters of Nursing. Learn how to prevent them and deal with them when they happen. Don’t give up on nursing because of this. You will get better in a day or two. Remember you’re in it for the long haul.
B. Social awkwardness about nursing
If you have any hope of leaving your house to do anything, you’re probably going to have to get comfortable with nursing outside your home. This can be really intimidating if you live in a place where nursing in public is not the norm. With a nursing cover, however, you can nurse anywhere discreetly and comfortably. I recommend practicing with your nursing cover at home so your baby gets used to it and you’re not trying to figure it out for the first time under pressure. (Again, your baby will likely be screaming and flailing around because she’s hungry, so this will add to the difficulty of getting the hang of your nursing cover, initially.)
Yes, it can be nerve-wracking the first few times. I’ll never forget our mommies group meeting at Starbucks for the first time with our 2-month-old babies. Some of the babies were getting hungry, but everyone was waiting for someone else to be the first one. Finally, Sara put on her nursing cover and said, “Let’s do this.” Everyone breathed a collective sigh of relief and gradually followed suit. Boy, we must have been quite a sight! After that though, it was easy. Nobody gave it a second thought. And no one else around us looked or cared.
You think everyone is staring at you, but they’re really not. And if they ARE… fuck ‘em. And believe me, by the time you have your 2nd baby, you won’t even think twice about this.
If you’re really shy and just can’t do it, you can always just pump and fill a bottle and bring it along. The downside is that you now have to warm up the milk somehow, depending on your baby. Lucie would never take a bottle unless it was very warm, but every baby is different. (BTW, the sooner you get your baby used to cold milk, the better.)
Once you get used to nursing anywhere, you’ll have a great sense of empowerment.
After your baby is a few months old, this is a moot point because he won’t have to feed as often and it will (hopefully) be more easy to plan your outings around feedings (but then you’ll have naptime, LOL).
C. Lack of confidence/support
My baby isn’t getting enough milk – gah!
I can’t tell you how many times I’ve heard this. Yes, it’s extremely worrisome to think you aren’t making enough milk for your baby, and this kind of self-doubt can really mess with your head.
There are a few things that can help put your mind at ease:
- You can always PUMP your milk to see exactly how much you are producing. Is it enough? Then feed your baby from a bottle. Don’t worry about nipple confusion unless you do this very frequently. Your baby is getting enough if he isn’t freaking out after finishing a nursing session and has 5-6+ wet diapers in a 24-hour period (after the first week).
- Consider a nursing supplement — the jury is still out (sort of), but there are a number of safe and/or delicious options that might help. (There are also other strategies you can try to boost your milk supply.)
- You CAN augment with formula if you really need or want to. The purists will say NO! Don’t do this, but – oh my gawd – isn’t this SO MUCH BETTER than stressing about your baby starving? We have to be reasonable — and getting nutrients to baby is the number one priority here. The key is, if you give formula, YOU MUST PUMP if you want to maintain/boost your supply. If you’re trying to increase your supply, pump for a few minutes AFTER you run dry.
Pitfall: The slippery slope begins when moms start giving their babies formula and then DON’T pump. Do this a few times and you will, I promise you, diminish your supply. Don’t fall into this trap. Have someone remind you to pump if you are feeling too bleary-eyed and brain dead. Or don’t, and that’s cool too.
The Big 3 Hairy Monsters of Breastfeeding
I don’t know many moms who have not dealt with at least one of these issues at some point in their nursing careers. Know how to recognize the symptoms so you can treat it quickly to minimize your angst.
1. Thrush
Thrush is a yeast infection of the nipple and/or breast. It’s the result of a fungus that thrives on milk on the nipples and/or in the milk ducts. Your baby can get it too. In fact, you can pass it back and forth to each other (sweet!).
The hallmark symptom of thrush is red, shiny, burning nipples. You may also experience shooting pains during or after a feeding, which may indicate a ductal invasion–> this is kinda bad news. You may also have nipple or breast pain when you are (correctly) using a pump.
Many, many, many nursing mothers get thrush, especially if you are already prone to yeast infections.
In your baby, look for a shiny or “mother of pearl” look inside the cheeks. There may be creamy, white patches that cannot be wiped off on the inside of the mouth, along the inside of the gums, inside of the cheeks, roof of mouth, or tongue. It may also spread to the diaper area. “Diaper rash” that doesn’t respond to regular rash cream, but responds to anti-yeast cream is a yeast infection. Your baby may also be completely asymptomatic.
How to Treat
You can run down to your OB’s office, but honestly, most women try to treat it at home first. You can use regular anti-yeast cream from the drugstore, such as Monistat or Lotrimin AF. Apply this to your nipple before your longest stretch of sleep (which is hopefully at night) and BE SURE TO WIPE IT OFF BEFORE NURSING. Do this for several days and if it doesn’t clear up, see your doc.
When the infection is ductal, causing shooting or stabbing pains within the breast, things get a little more complicated. Your doctor will probably prescribe Difulcan and may even suggest a low-yeast diet. Some ductal infections can be really, really gnarly and hard to beat.
Nursing can (and should) be continued through treatment.
Prevention
The best way to prevent thrush is by keeping your nipples dry. Change your nursing pads promptly when they become wet (this is also why I hate LilyPadz). Also, make yogurt (with acidophilus) a part of your daily diet. Acidophilus helps keep yeast growth in check.
Other Notes:
- *It’s SUPER important to be neurotic about hygiene if you (and/or your baby) develop thrush — threat that sh*t like lice. It’s very contagious, so make sure to wash your hands carefully, wash your clothes or nursing covers carefully, pumps/bottles, anything that goes in your baby’s mouth, etc.
- La Leche League suggests limiting carbs and sugars, especially processed/refined ones, as these foods seem to interfere with recovery.
- Don’t store any pumped/expressed milk while you or your baby have thrush — it could potentially reinfect.
2. Blocked ducts
Jeez, I could write a book on this topic. I get them so bad that I have scoured every nook and cranny on the internet, talked to lactation consultants, doctors, other moms… you name it. When you get blocked ducts, you can get a little desperate for pain relief.
A blocked duct can really be felt when you bend over at the waist and the weight of your breasts falls forward. I don’t know why but this position always makes them hurt.
A blocked duct presents as a painful, swollen hard mass in the breast, sometimes accompanied by surface redness.
A clogged duct is caused by insufficient drainage of your milk, either because of engorgement, a bad latch, missed feedings, wearing a bra, bathing suit, or even a baby carrier that’s too tight around your breasts, sleeping in the wrong position, or by sneezing (ok, that one’s a joke).
Sometimes, you can feel the actual blocked duct itself and sometimes, like in my case, the whole area or an entire side of the breast is sore and you can’t pin it to a specific location. This is really frustrating. Sometimes the whole damn breast feels like a clogged duct! (Confession: I threw a book against the wall one time I was in so much pain. It takes a lot for me to throw a book against the wall…)
Bad news first: There isn’t anything your doc can do for you, except perhaps prescribe a painkiller to get you through the painful “massage” you’re about to do. (You can also take an OTC med like ibuprofen or acetaminophen.) You have to work these bad boys out on your own. It sucks, but here’s how:
- Prepare a heating pad for the affected breast. Apply heat for about 5 minutes *right before* nursing. (Yes, this whole shindig goes down while you’re breastfeeding.) (Also, if you don’t have a heating pad, you can use a washcloth with hot water.)
- Now that you’ve applied heat to get the blood circulating, get the baby latched on (owwww, I know). You want her CHIN to be pointed in the general direction of the affected duct. Do acrobatics if you must.
- Your best weapon is the SUCK (for lack of a better word) from your baby’s sucking. Yes, it can be incredibly painful! It’s important for her suck to draw from the affected duct(s). You gotta bite the bullet on this one, my dear. You need to keep nursing or else you’re really screwed.
- Right after nursing, you want to use massage to try to work it out. Think about kneading bread dough. You can also try to do this while you are nursing, but the logistics are difficult — you need about four arms for it to work properly. First, apply some lotion or olive oil to the area to make it slippery. Then, you want to massage the area of pain *toward* your nipple, as though to push the milk toward the nipple. Ouch, I know I know I know. Do it for as long as you can stand it.
- Pat yourself on the back and take a deep breath because that hurt like bloody hell. Now go put a cold cabbage leaf on your breast – any variety will do. It’s very Adam and Eve-esque. (Note: overuse of cabbage leaves can decrease milk supply. Also, note that cabbage contains sulfa, so if you have an allergy to sulfa, don’t use or ask your doctor.)
Repeat this (^^) several times a day until you work it out.
Two more important things:
- 1) You need to take your lecithin, (1,200 mg) 3 or 4 times a day with a blocked duct. Lecithin has emulsification and lubricant properties – it’s like Drain-O for your milk ducts. Taking too much can make you nauseated, dizzy, and depressed (no joke), so don’t O/D on it.
- Also, 2) you need to drink boatloads of water to thin everything out. Fill up the huge 32 oz water jug that you stole from the hospital and drink several refills per day. Stay hydrated. Are you feeling like a camel yet?
Desperation
Didn’t work? Sigh. Yeah, me neither. I have 2 tricks for desperate souls. You will feel ridiculous, but this technique works really well:
You need to nurse your baby while hovering.
That’s right, you will be on all fours and down on your elbows so that your bubbies are dangling down. Do this on a soft place like your bed – it’s actually not that bad. There is something about the gravity in this position that helps break up the blockage. You can also do this while pumping if nursing is too painful, it just won’t be quite as effective.
The second thing I learned from a great lactation consultant… for a freakishly-stubborn blockage, you can use vibration to work it out. You can seek out an ultrasound tech at a physical therapy office, or you can try a Sonicare toothbrush or anything that vibrates (ahem). Lube it up, press the vibrator as hard as the pain allows, pushing toward the nipple. This worked on stubborn blockages for me. Mine always took several days to resolve, which is very uncommon. Stay the course. You’ll beat them, I promise.
*One last thing to note is when you finally do break up the blockage, you may not be able to tell until the next morning. If you still feel the blockage after an extensive workout session, don’t be too discouraged. You may not know that you succeeded until a little later.
3. Mastitis
As if the pain of blocked ducts wasn’t bad enough, many women will go on to develop mastitis. I wrote this bit after recovering from a giant blocked duct situation, which then caused mastitis. It was so awesome and fun. I got to spend the whole weekend in bed with a major headache and fever.
Puerperal mastitis is the inflammation of the breast associated with breastfeeding or weaning. It’s thought to be caused by blocked milk ducts, excessive supply, and engorgement. It’s most common in the fourth trimester, and it’s relatively common among nursing moms: about 1 in 10 will get it. Symptoms usually appear suddenly and include:
- Breast tenderness, warmth to the touch, or swelling
- A fever of 101 F or greater
- Headache
- General malaise or feeling ill
- Pain or a burning sensation continuously or while breastfeeding
- Skin redness, often in a wedge-shaped pattern
A fever is really the hallmark of mastitis. If you have plugged ducts and you have a fever, you probably have mastitis. You don’t have the flu. The perpetrator is usually the bacteria staphylococcus aureus (i.e., staph), which enters your system through the nipple or a skin lesion. Your doctor will likely prescribe an antibiotic, although it can go away on its own (mine did). Delayed or inadequate treatment may lead to the formation of an abscess within the breast. An abscess is… you don’t want to know. Google it. It’s gnarly and you don’t want it. Don’t delay in talking to your doctor.
*Note also: keep nursing. Sorry : /
So there you have it: the 3 big gremlins you can get while nursing. I think of this as the “nursing tax”… it’s just a price that you’ll (probably) pay to provide your baby with the best food in the world (although feel free to curse me while you are suffering).
Resources:
- KellyMom
- La Leche League
- Breastfeeding Basics
- The Breastfeeding Companion
- The Womanly Art of Breastfeeding– book
Related:
Next: Postpartum Depression