The Truth about Prenatal Vitamins
Do I really need prenatal vitamins – and if so, which one is “the best?”
We get a lot of readers asking this question… and what we uncovered might surprise you –
Prenatal Vitamins: “Optional Nostrums”
In a nutshell:
The only components of a prenatal multivitamin that pregnant women actually, definitively “need” are folic acid, (maybe) iron, and (probably) vitamin D — but virtually everyone takes (and recommends) a prenatal multivitamin.
Jump ahead to learn more about:
- Folate
- Vitamin D
- Iron
- Calcium and DHA
- Prenatal multivitamins
- Supplement Recommendations (aka product picks)
First — here are the “official recommendations” on prenatal vitamins from the three public health organizations we typically look to for advice ~
- The American College of Obstetricians and Gynecologists (ACOG) suggests taking a daily prenatal multivitamin (though it has no official committee opinion squarely on vitamin supplementation during pregnancy, and formerly it recommended daily folic acid and iron alone).
- The Centers for Disease Control (CDC) only calls for folic acid.
- The World Health Organization (WHO) recently changed its recommendations (in 2020) to advise for multivitamins that include folic acid and iron. (The caveat with the WHO is that the evidence for this new guideline is strongest in low- and middle-income countries (aka, not countries like the US); prior to 2020, the WHO only recommended folic acid and iron.)
What You Really Need: Folate
The evidence and formal guidelines from the most reputable medical associations on the planet make one thing crystal clear: folate (vitamin B9) and the synthetic version (folic acid) reduce the risk for neural tube defects – like anencephaly and spina bifida – by a lot.
Pregnant women need more folate – about 50% more – than non-pregnant women, and it’s a very good idea to begin taking folic acid pre-conceptually. Here’s why: folate is most important in the very first days of pregnancy, right after conception, before an embryo’s neural tube has closed — which occurs about 28 days after conception (approximately six weeks after your LMP, and before many women even realize they are pregnant). A mere two weeks after peeing on a stick is how long you have before the neural tube closes…
… no pressure.
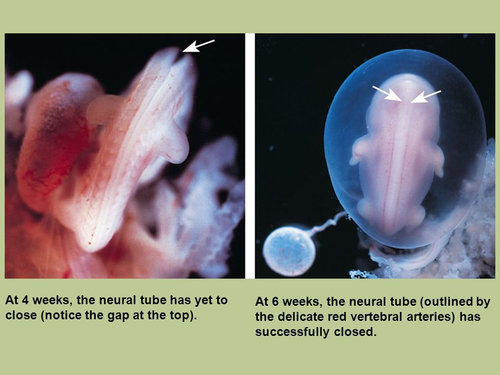
Taking folic acid after this point won’t help prevent neural tube defects, but all recommendations still call for folic acid at least through the first trimester, perhaps out of an abundance of caution, mixed with a lack of confidence in knowledge of pregnancy timing.
Note: it’s also critically important to avoid elevation of the mother’s body temperature during this “neural tube closing” time period, as hot tubs, saunas, fever, etc., have been linked to increased risk of neural tube defects.
Good news: In the U.S. and most other western countries, grain products have been fortified with folic acid since the 1990s, and folate deficiency has since become relatively unusual. Even without a supplement, most women are still obtaining at least some folic acid through their diet (which, ironically, may be one of the only known benefits of eating processed foods).

To Summarize on FA~
Guidelines advise taking 400 micrograms (mcg) of folic acid daily, starting at least one month prior to conception and continuing at least through the first trimester. Avoid hot tubs and otherwise elevating your body temperate during the first trimester, especially in the first 6 weeks.
As you might surmise, the first trimester is the most sensitive/critical period for a developing fetus.
What About the Other Stuff?
Only a handful of other prenatal multivitamin components have been individually studied, and trying to isolate their individual effects is like trying to find a needle in a haystack.
At this point, research indicates that vitamin C, vitamin E, and iodine (probably) confer no benefit to pregnant women or babies, and routine supplementation is not required. The evidence regarding vitamin D and iron, on the other hand, is more intriguing (if somewhat controversial). In the last year or two, more research is coming out showing that multivitamin supplementation does confer benefits for women in low- and middle-income countries.
Let’s have a look.
Vitamin D
In the U.K. and Canada, pregnant women are advised to take vitamin D, but ACOG (in the U.S.) does not specifically call for it. (Of course, most women’s prenatal multi already includes vitamin D…)
There may not be a ton of solid research specifically linking vitamin D to improved pregnancy and birth outcomes, but a wealth of research shows that many American women (especially pregnant and nursing women) are vitamin D deficient – or insufficient – to begin with.
In some studies of first-world people, deficiency levels reached as high as 97% (gasp) of the population – and most studies agree that 50 – 70% of the U.S. population is vitamin D deficient.
Who cares about D? Why is it so important?
Modern-day humans evolved near the equator, and vitamin D receptors are in the nuclei of nearly every cell in our bodies. As humans migrated further and further from the predominant fuel source for vitamin D (the sun!), their need for sunlight did not diminish.

Vitamin D is essential for human life and wellbeing. It works as a kind of light switch in your body, turning on or off genes and processes that your body needs to maintain health and fight infection. Vitamin D prevents autoimmune disease by promoting T cells, which differentiate between outside invaders and your own cells.
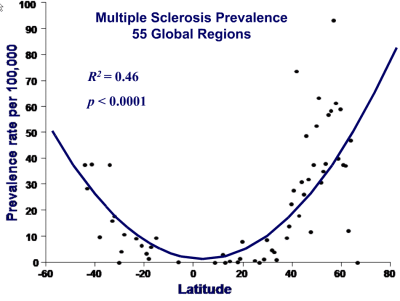
Generally speaking, moving farther away from the equator, people tend to have correspondingly lower vitamin D levels and higher levels of morbidity and mortality (see presentation here). This could help explain why populations who live near the equator have low rates of diseases like MS, type 1 diabetes, autism, and asthma, among many others.
“But I get a lot of sun” . . . do you? Unless you work outdoors or lounge by the pool on a daily basis, you probably don’t, especially in the winter months and with the sunscreens that have become ubiquitous in our skin care products. The problem is that sunscreens are very good at blocking out UV-B rays, which provide us with vitamin D and are less damaging to the skin, and very bad at blocking out UV-A rays, which inflict deeper cellular damage, like melanoma.
Breastfed Babies
Vitamin D deficiency is also of special concern for lactating women and their babies, since exclusively breastfed babies get their vitamin D solely from breastmilk (in the U.S. and Canada, all infant formula is required to be fortified with vitamin D).
Breastmilk in non-equatorial climates is almost universally deficient to the extent that the Committee on Nutrition of the American Academy of Pediatrics recommends added maternal vitamin D intake as well as daily infant vitamin D supplements.
Vitamin D for Infants
According to the AAP and the CDC, breastfed infants should take a liquid vitamin D supplement of 400 IU /mL per day, starting within a few days after birth and continuing until the baby is weaned completely to fortified formula or vitamin-D fortified whole milk. This tasteless liquid supplement is administered with a medicine dropper (see recommendations below).
Better yet, mom can take a “nursing dose” of Vitamin D, which is enough to give you both enough D.

Thus, the foremost experts are concerned that the amount of vitamin D in most prenatals – 400 IU (international units) – is not nearly sufficient to meet women’s (or nursing babies’) needs. They suggest taking more – typically, 4,000-6,000 IU daily.
That approach seems reasonable – and it’s gaining traction. (There’s a wonderful clinical review Q&A piece on vitamin D if you’re interested.)
So far, no negative effects of vitamin D supplementation have been documented, and almost no one has vitamin D levels that are “too high.”
Given all the evidence emanating from respected researchers and scientific associations about the universality of vitamin D insufficiency among American women, as well as the general lifetime health benefits associated with maintaining optimal vitamin D levels, taking vitamin D beyond what’s contained in a prenatal may be a good habit to consider starting anyway.
Iron
Women need progressively more iron throughout pregnancy simply because of increased blood volume (more blood needs more iron). In fact, about 4 lbs of weight gain during pregnancy can be attributed just to the extra blood in your body (jeah), and pregnant women need about 27 mg of iron per day (more for vegetarians), compared to 18 mg for non-pregnant women.
As the placenta grows and blood volume amps up from trimester to trimester, iron needs increase correspondingly. Thus, women are more likely to be iron deficient later rather than earlier in pregnancy. Some estimates suggest that more than one third of pregnant women are iron deficient by the end of their pregnancies.
Iron deficiency can exert negative effects on your cognition, energy, and immune system. In essence: being low on iron can make you feel really crappy. It can also increase the risk of maternal and infant mortality, premature birth, and low birthweight.

Though there is no clear consensus on how much is needed, you can get a feel for the various recommendations; heavy meat-eaters will generally need less and vegetarians/vegans will need more (and perhaps, lots more…).
Technically not every woman needs supplementation, but since pregnant women as a group are more at-risk for deficiency, both ACOG and the WHO both recommend daily iron supplements in the context of a prenatal.
Side-effect Alert
Iron supplements can cause problems like nausea and constipation, which can be particularly rough in the throes of morning sickness.
Surviving morning sickness or hyperemesis gravidarum and the first trimester in general can be brutal; if iron is making it worse, you can always take a break and try again later on, especially since deficiency becomes more of a concern as pregnancy progresses.
Okay, so we’ve discussed what our findings consider the “Big 3“: Folate, Iron and “everyone needs Vitamin D anyway.”
What about….
Calcium
Pregnant women need about 1,000 mg of calcium daily, but there is no current consensus about routine calcium supplementation during pregnancy. Fortunately, the pregnant body actually absorbs more calcium to meet its own needs, especially in the second and third trimesters.
In women with low calcium intake (less than 500mg/day), supplementing with calcium is associated with a reduced risk for preterm delivery. For pregnant women with high blood pressure (hypertension), studies indicate that 1,000 mg daily calcium supplementation can reduce the risk of preeclampsia.

If you are concerned about your calcium intake (you’re dairy-free, for example), it’s reasonable to speak with your physician about a supplement of 600 – 1,000 mg.
DHA
Research suggests that DHA (or fish oil) supplements have no positive effects on maternal, fetal, or infant health. You can read about one such full study here.
DHA is clearly important for fetal maturation (more so in the second half of pregnancy than the first), but judging by the research the best way to get it is to eat fish!

In fact, the natural form of DHA, found especially in seafood, is associated with benefits such as a reduced risk of postnatal depression, heavier birth weight (by about 6 ounces), and longer gestational lengths (by about 4 days), but research on the effects of synthetic/processed DHA supplementation shows no such advantages.
Bottom line: Your best bet for optimizing omega-3 fatty acid intake is to eat fish 1-2 times per week, if you’re able. Salmon is a great choice because it has very low mercury levels and high DHA (and EPA) levels.
And finally —
Multi’s
Prenatal multivitamins seem to be the go-to for most, though most studies of 1st world populations suggest that multivitamins offer no benefits beyond those associated with folic acid and iron. One 2016 review announced that there was “no evidence to recommend that all pregnant women should take prenatal multi-nutrient supplements.” (In underdeveloped countries where deficiencies and malnutrition are more widespread, prenatal multivitamins appear to offer more benefits.)

Bottom Line
Based on the available evidence, women should feel like they have a choice regarding whether to take a prenatal multivitamin. If it’s not up your alley, there is more than enough research to back your decision (just make sure you take folic acid and confirm that your iron and vitamin D levels are normal).
That said, many women are probably going to want to keep taking prenatals, and that’s OK! Just know that many of them don’t contain iron (at all) and most only contain a fraction of the recommended vitamin D. In other words, you might have to (or want to) supplement anyway.
If you’re interested in a deeper dive on the history & evolution of prenatal vitamins, the first chapter of my book Carrying On is exactly that…
Here are a few final things to be mindful of:
1. More is not better. Excessive doses of individual vitamins or minerals can be dangerous. If you consume separate supplements, make sure that you aren’t exceeding upper tolerable limits. You can check the pregnancy-specific upper tolerable intake levels here.
2. It really doesn’t matter which brand you take. Though there are likely vast differences in quality across products and brands at large in the supplement industry (remember: it’s not a regulated industry), there’s no real way of knowing which supplements are “better” than others. As Dr. Anna Sfakianaki, an obstetrician and associate professor at Yale University, explains: “the differences between prenatal vitamins are slight, and no particular vitamin can be recommended over another.” Bottom line: don’t obsess over it.
3. Prenatals can be difficult to stomach (predominantly due to their iron content), especially for women suffering from morning sickness. Professionals recommend taking them at night, with food, to ease discomfort. For some women this helps, while for others, it provides no relief. If you want to try different brands or blends to see if any work for you, you can . . . or you could give yourself a break and hold off on prenatals altogether until you start feeling better.
4. Some subgroups of pregnant women might want to give special consideration to a prenatal multivitamin and/or vitamin D or iron. Women who are vegetarian, vegan, at-risk for vitamin-D deficiency (which could potentially include all pregnant women), suffering from eating disorders, smoking, or taking certain prescription medications that might interfere with vitamin absorptions may have an increased risk for specific shortages. If you fall into any of these groups, talk to your doctor.
Product Options
Every person’s body is going to handle, digest, and absorb vitamin supplements differently, so you might find that some work better for you than others. Here are some we recommend based on our personal experiences and hundreds (and sometimes thousands) of user reviews. (Skip ahead to multivitamin picks.)
**Note: Prenatals are FSA/HSA eligible — use those tax free dollars!
Folic Acid Only Supplements
Nature Made Folic Acid, 400 mcg ~$5 for 250
Nature Made’s highly rated folic acid supplement is verified by the U.S. Pharmacology Convention, which signifies that it passed through stringent quality and safety testing. The tablets are small and uncoated.
Suggested use: take one tablet daily with a meal.
Pink Stork Folate, 1,000 mcg ~ $24 for 60 capsules
Though folic acid and folate are terms that are often used interchangeably, they are not the same thing. Pink Stork (and some others on the market) contains actual folate (vs. folic acid). This is ideal for the large percentage of the population suffering from the MTHFR genetic mutation (an inability for the body to convert folic acid into the usable form, methylfolate).
Many moms with morning sickness or HG say it’s easy to take (and keep down!). The capsules are small, easy to swallow, and have no taste or odor. *Also available in liquid form.
Suggested use: take one capsule daily with water.
Iron Only Supplements
NOW Iron, 18 mg ~ $8 for 120 capsules
Users say this very highly-rated iron supplement is well tolerated and non-constipating. This iron is provided in the form of iron bisglycinate and is gluten, wheat, and dairy-free. Important note: the recommended dietary intake of iron during pregnancy is 27 mg, and NOW Iron only contains 18 mg. Thus, this is a good one if you are getting other good sources of iron in your diet.
Suggested use: take one capsule daily with a meal.
Solgar Gentle Iron, 25 mg ~ $20 for 180 capsules
This highly-rated “gentle iron” is easy to take and provides you with 25 mg of iron, which is more than the NOW brand (above). Users report no effects, even on an empty stomach, and report it’s non-constipating and easily absorbed.
Suggested use: take one capsule daily with a meal.
Vitamin D
NatureWise Vitamin D3 – 5,000 IU ~ $14 for 360 (one year’s worth)
This is the top-rated, best-selling D Vitamin on Amazon. The softgels are very easy to swallow and digest.

Best Nest Advanced Vitamin D3 Drops 2,000 IU Per Drop ~ $20, 1 Oz
As an alternative to pills, you can take vitamin D3 from a liquid dropper. These drops are odorless and tasteless, and you can take them straight or mix into a smoothie or any other kind of beverage (or food, for that matter). With 2,000 IU per drop, you can decide if you want to take 2000, 4000, or 6000 IUs. (One drop is 2000 IU and each bottle contains ~1400 drops.)
Vitamin D For Infants and Children
Carlson Labs Super Daily D3, 400 IU ~ $12 for 10.3 ml (365 drops)
One drop per day is all it takes to give your infant or child their recommended dose of Vitamin D. You can add a drop to expressed milk or drop onto nipple just before feeding. Sounds weird, but… it works!
Prenatal Multivitamins
Prenatal vitamins can simplify your life — these ones contain iron, folic acid, some vitamin D, and are highly-rated and easy to digest. (Listed in order of increasing price.)
Nature Made Prenatal ~ $15 for 250 tablets
We chose this one for its simplicity: just one pill a day gives expectant mamas their full quota of folic acid and iron. Not all prenatals pack such a powerful punch – especially “one-capsule-a-day” brands. Bonus: moms say it’s easy to swallow and doesn’t make them nauseous. This brand is verified by the USP.
Suggested use: take one tablet daily with a meal.
New Chapter Whole-Food Prenatal ~ $28 for 96 tablets
This prenatal is ideal for those having trouble with nausea and digestive problems. With this 3-a-day vitamin, the nutrients are spread out, which helps keep nausea at bay — and you don’t have to take it with food. If you aren’t having digestive issues, it may be easier to stick with a one-a-day vitamin (obvi).
We also like that is has 100% RDA of non-constipating iron (not all prenatal multis offer this!) and real folate (actual folate, not folic acid). New Chapter Prenatals are also non-GMO project verified, vegetarian, kosher, gluten-free and sugar-free. Fancy!
Suggested use: take three tablets daily anytime, even on an empty stomach.
So simple, as you can see! LOL
Thanks for sticking with us – and good luck!
See also (sources);
World Health Organization, WHO Recommendations on Antenatal Care for a Positive Pregnancy Experience, 2016, xi.
Luz Maria De-Regil et al., “Effects and Safety of Periconceptional Oral Folate Supplementation for Preventing Birth Defects,” in Cochrane Database of Systematic Reviews, ed. The Cochrane Collaboration (Chichester, UK: John Wiley & Sons, Ltd, 2015), doi:10.1002/14651858.CD007950.pub3; Roy M. Pitkin, “Folate and Neural Tube Defects,” The American Journal of Clinical Nutrition 85, no. 1 (January 1, 2007): 285S–288S; Pietro Cavalli, “Prevention of Neural Tube Defects and Proper Folate Periconceptional Supplementation,” Journal of Prenatal Medicine 2, no. 4 (2008): 40–41; Breige McNulty et al., “Impact of Continuing Folic Acid after the First Trimester of Pregnancy: Findings of a Randomized Trial of Folic Acid Supplementation in the Second and Third Trimesters,” The American Journal of Clinical Nutrition 98, no. 1 (July 2013): 92–98, doi:10.3945/ajcn.112.057489.
A. Milunsky et al., “Maternal Heat Exposure and Neural Tube Defects,” JAMA 268, no. 7 (August 19, 1992): 882–85.
World Health Organization, WHO Recommendations on Antenatal Care for a Positive Pregnancy Experience, xii; Kimberly B. Harding et al., “Iodine Supplementation for Women during the Preconception, Pregnancy and Postpartum Period,” The Cochrane Database of Systematic Reviews 3 (March 5, 2017): CD011761, doi:10.1002/14651858.CD011761.pub2; “Vitamin E Supplementation in Pregnancy | Cochrane,” accessed June 6, 2017, /CD004069/PREG_vitamin-e-supplementation-pregnancy.
Philip J. Steer, “Is Vitamin D Supplementation in Pregnancy Advisable?,” The Lancet; London 381, no. 9884 (June 22, 2013): 2143.
Amanda Schaffer and Carl Wilson, “Essential Nutrient,” Slate, August 24, 2004; Adit A. Ginde et al., “Vitamin D Insufficiency in Pregnant and Nonpregnant Women of Childbearing Age in the United States,” American Journal of Obstetrics and Gynecology 202, no. 5 (May 2010): 436.e1, doi:10.1016/j.ajog.2009.11.036; Megan L. Mulligan et al., “Implications of Vitamin D Deficiency in Pregnancy and Lactation,” American Journal of Obstetrics and Gynecology 202, no. 5 (May 1, 2010): 429.e1-429.e9, doi:10.1016/j.ajog.2009.09.002; Donna D. Johnson et al., “Vitamin D Deficiency and Insufficiency Is Common during Pregnancy,” American Journal of Perinatology 28, no. 1 (January 2011): 007–012, doi:10.1055/s-0030-1262505; The American College of Obstetricians and Gynecologists, “Committee Opinion Number 495: Vitamin D: Screening and Supplementation During Pregnancy,” July 2011; Ivor Cummins, D Is for Debacle – The Crucial Story of Vitamin D and Human Health, accessed June 14, 2017.
Bruce W Hollis, “Vitamin D Requirement During Pregnancy and Lactation,” Journal of Bone and Mineral Research 22, no. S2 (December 1, 2007): V39–44, doi:10.1359/jbmr.07s215; Janyne Althaus, “Clinical Review: Vitamin D and Pregnancy: 9 Things You Need to Know,” accessed June 14, 2017.
Ginde et al., “Vitamin D Insufficiency in Pregnant and Nonpregnant Women of Childbearing Age in the United States,” 436.e5; Althaus, “Vitamin D and Pregnancy”; Office of Dietary Supplements National Institutes of Health, “Vitamin D,” accessed June 14, 2017; Cummins, D Is for Debacle – The Crucial Story of Vitamin D and Human Health.
Tara Haelle and Emily Willingham, The Informed Parent: A Science-Based Resource for Your Child’s First Four Years (New York: TarcherPerigee, 2016), 4; National Institutes of Health Office of Dietary Supplements, “Iron,” accessed June 15, 2017.
Thomas H. Bothwell, “Iron Requirements in Pregnancy and Strategies to Meet Them,” The American Journal of Clinical Nutrition 72, no. 1 (July 1, 2000): 257S; Office of Dietary Supplements, “Office of Dietary Supplements – Dietary Supplement Fact Sheet.”
John L. Beard, “Effectiveness and Strategies of Iron Supplementation during Pregnancy,” The American Journal of Clinical Nutrition 71, no. 5 (May 1, 2000): 1289S.
World Health Organization, United Nations Children’s Fund, and United Nations University, “Iron Deficiency Anaemia: Assessment, Prevention, and Control: A Guide for Programme Managers,” 2001, 7, 9; Office of Dietary Supplements, “Office of Dietary Supplements – Dietary Supplement Fact Sheet.”
Andrea N. Hacker, Ellen B. Fung, and Janet C. King, “Role of Calcium during Pregnancy: Maternal and Fetal Needs,” Nutrition Reviews 70, no. 7 (July 2012): 397–98, 401, 406, 400, doi:10.1111/j.1753-4887.2012.00491.x.
Maria Makrides et al., “Effect of DHA Supplementation During Pregnancy on Maternal Depression and Neurodevelopment of Young Children: A Randomized Controlled Trial,” JAMA 304, no. 15 (October 20, 2010): 1675, doi:10.1001/jama.2010.1507; Katharine D. Wenstrom, “The FDA’s New Advice on Fish: It’s Complicated,” American Journal of Obstetrics and Gynecology 211, no. 5 (November 1, 2014): 475–478.e1, doi:10.1016/j.ajog.2014.07.048; Jacqueline F. Gould et al., “Seven-Year Follow-up of Children Born to Women in a Randomized Trial of Prenatal DHA Supplementation,” JAMA 317, no. 11 (March 21, 2017): 1173–75, doi:10.1001/jama.2016.21303.
James A Greenberg, Stacey J Bell, and Wendy Van Ausdal, “Omega-3 Fatty Acid Supplementation During Pregnancy,” Reviews in Obstetrics and Gynecology 1, no. 4 (2008): 162–69.
BMJ Publishing Group, “Vitamin Supplementation in Pregnancy,” Drug and Therapeutics Bulletin 54, no. 7 (July 1, 2016): 83, doi:10.1136/dtb.2016.7.0414.
Duckworth, Mistry, and Chappell, “Vitamin Supplementation in Pregnancy,” 176; Anna K. Sfakianaki, “Prenatal Vitamins: A Review of the Literature on Benefits and Risks of Various Nutrient Supplements,” Formulary Watch, January 13, 2013; R. Douglas Wilson et al., “Pre-Conceptional Vitamin/Folic Acid Supplementation 2007: The Use of Folic Acid in Combination With a Multivitamin Supplement for the Prevention of Neural Tube Defects and Other Congenital Anomalies,” Journal of Obstetrics and Gynaecology Canada 29, no. 12 (December 1, 2007): 1004, doi:10.1016/S1701-2163(16)32685-8.
Sfakianaki, “Prenatal Vitamins: A Review of the Literature on Benefits and Risks of Various Nutrient Supplements.”
Nils Hovdenak and Kjell Haram, “Influence of Mineral and Vitamin Supplements on Pregnancy Outcome,” European Journal of Obstetrics & Gynecology and Reproductive Biology 164, no. 2 (October 1, 2012): 131, doi:10.1016/j.ejogrb.2012.06.020; Sfakianaki, “Prenatal Vitamins: A Review of the Literature on Benefits and Risks of Various Nutrient Supplements”; Steer, “Is Vitamin D Supplementation in Pregnancy Advisable?,” 2145; Daphne Adler, Debunking the Bump: A Mathematician Mom Explodes Myths about Pregnancy (CreateSpace Independent Publishing Platform, 2014), 133.








